Our Comprehensive Guide to Eczema and Dermatitis
Before we go any further would you like to take the test to see which products are suited to your skin type?
Your Natural Solutions
Our Comprehensive Guide to Eczema and Dermatitis - Your Path to Healthier Skin
Dive into our comprehensive guide on Eczema and Dermatitis, two of the most common chronic skin conditions impacting millions of individuals around the world.
Although the exact cause of eczema remains unclear, it is thought to be influenced by a combination of genetic, allergic, and environmental factors. Eczema often presents as a red, itchy, and inflamed rash, causing both discomfort and self-consciousness.
Various forms of eczema exist, including atopic dermatitis, contact dermatitis, seborheic dermatitis and xerotic dermatitis.
Numerous triggers can exacerbate eczema symptoms, such as stress, harsh detergents or soaps, woolen clothing, and extreme temperatures. In some cases, food allergies or intolerances may also provoke flare-ups. Identifying and avoiding these triggers is essential for managing eczema symptoms and preventing outbreaks.
Living with eczema can be challenging, but with proper care and a focus on natural and alternative approaches, individuals can find relief and maintain healthy skin.
Explore this page for more information, resources, and support on living with eczema and dermatitis using natural methods.
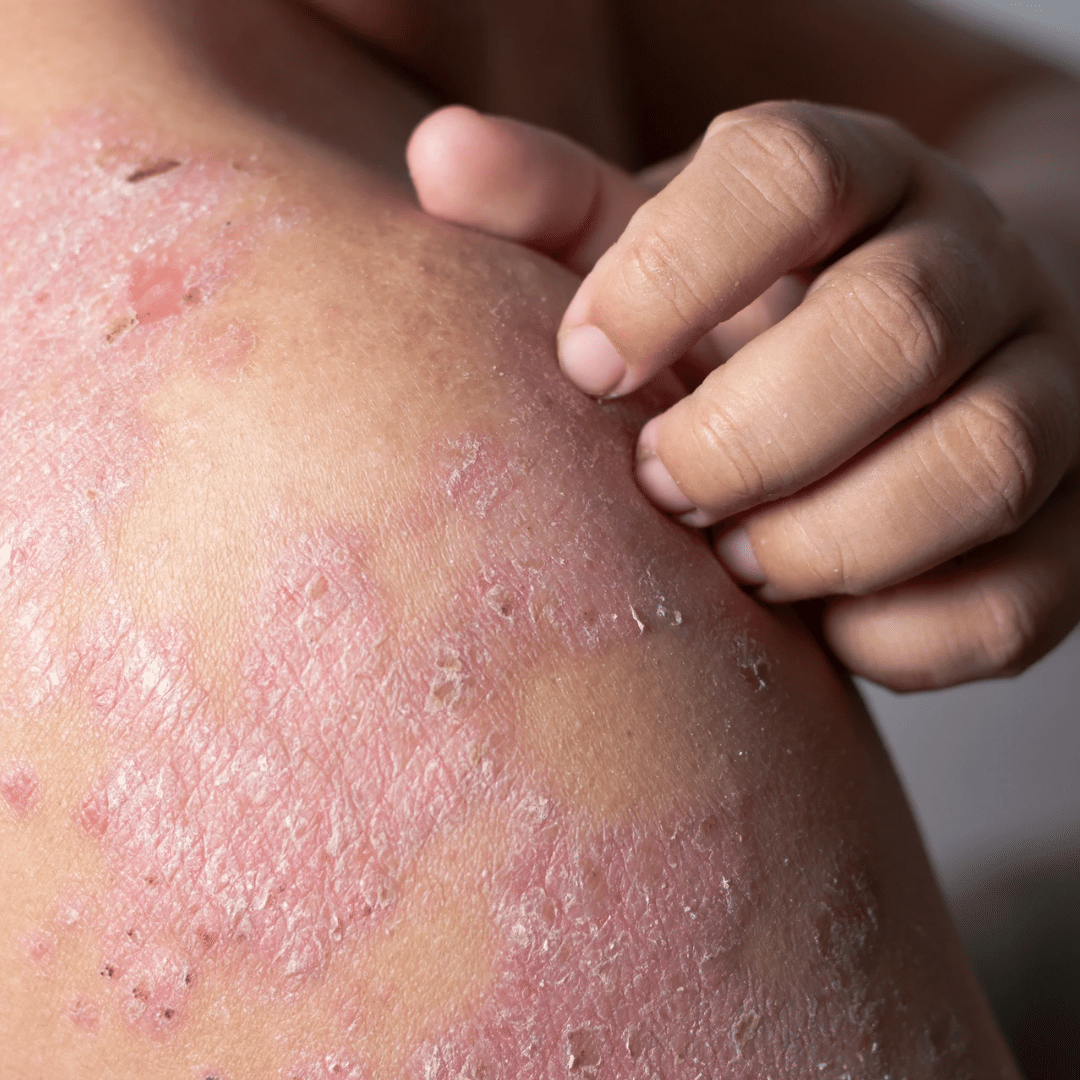
ATOPIC DERMATITIS
Atopic dermatitis, also known as eczema, is a chronic skin condition characterized by inflammation, redness, itching, and dryness.
It typically occurs in individuals with a genetic predisposition to developing allergies and is more common in children, although it can affect people of all ages.
Atopic dermatitis is often associated with other atopic (allergic) conditions, such as asthma and hay fever.
The exact cause of atopic dermatitis is not fully understood, but it is believed to involve a combination of genetic, immune system, and environmental factors.
People with atopic dermatitis often have a weakened skin barrier, making it easier for allergens and irritants to enter the skin and trigger an immune response.
Symptoms of atopic dermatitis can vary in severity and include:
- Itchy skin
- Red, inflamed patches of skin
- Dry, cracked, or scaly skin
- Small, fluid-filled blisters that may ooze and crust over
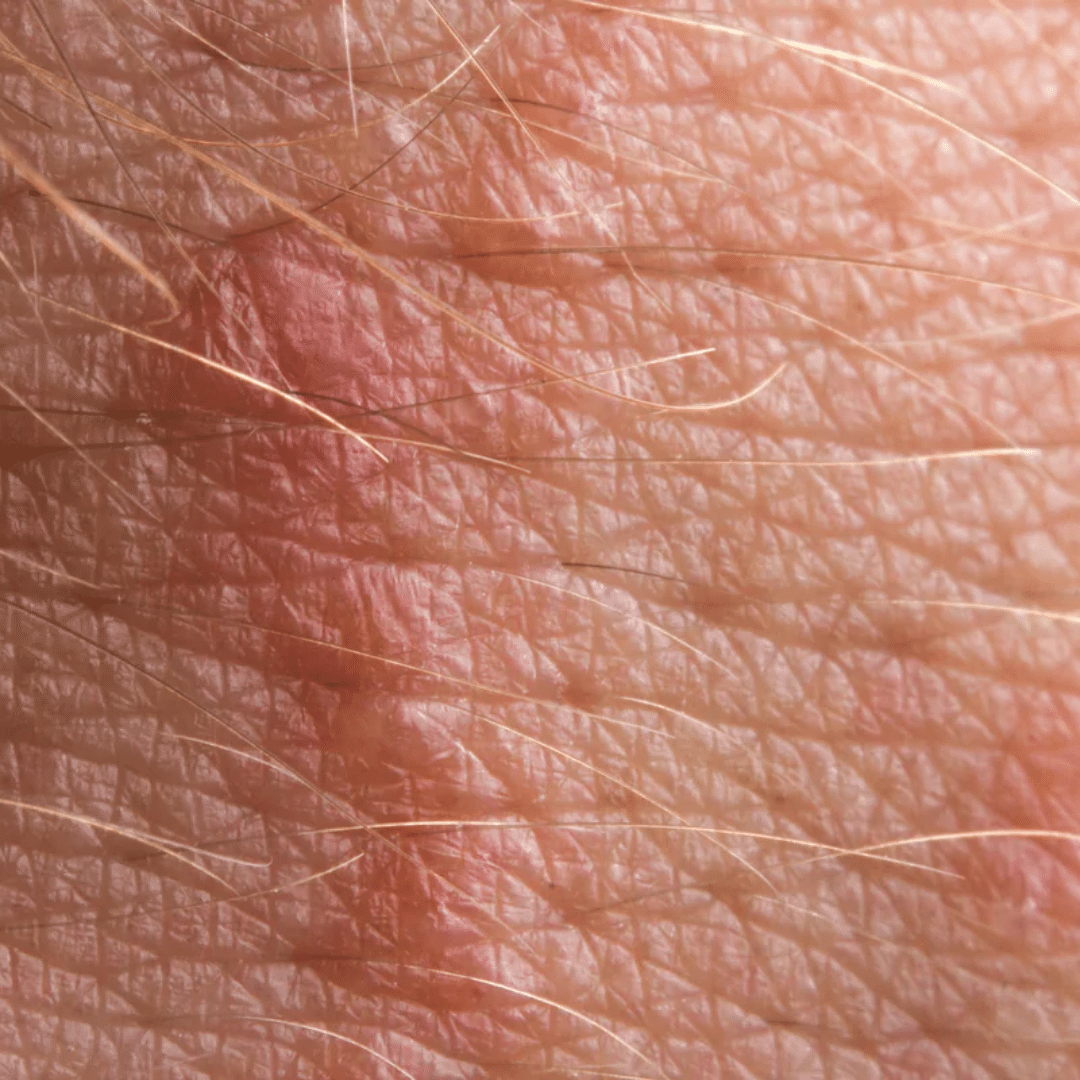
CONTACT DERMATITIS
Contact dermatitis is a type of skin inflammation that occurs when your skin comes into contact with a substance that either causes irritation or triggers an allergic reaction.
It usually presents as a red, itchy rash on the skin.
There are two main types of contact dermatitis:
Irritant contact Dermatitis:
This is the more common form and occurs when the skin comes into contact with an irritating substance, such as soap, detergent, or certain chemicals.
It can also be caused by environmental factors like cold or heat, and it usually affects people with sensitive skin or those who have frequent contact with irritants due to their occupation.
Allergic contact dermatitis: This form is caused by an immune system reaction to an allergen, such as poison ivy, nickel, or latex.
The allergic reaction can occur after just one exposure or develop after repeated exposures to the allergen.
It is important to identify and avoid the irritants or allergens causing the reaction.
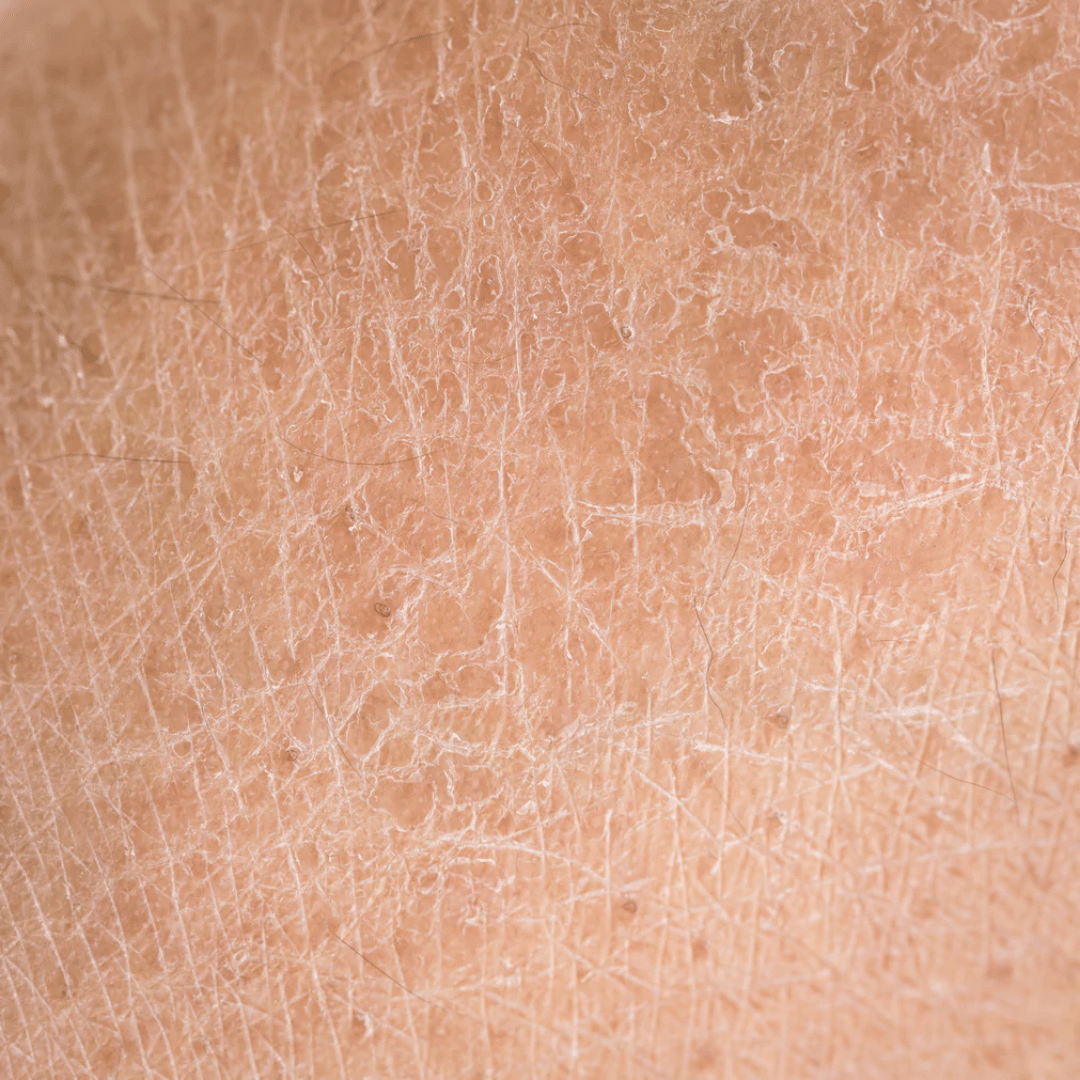
XEROTIC DERMATITIS
Xerotic dermatitis, also known as eczema craquelé or asteatotic eczema, is a type of dermatitis that occurs when the skin becomes excessively dry and loses its natural moisture.
This dryness can lead to the development of fine cracks or fissures on the skin's surface, giving it a "crazed" or "cracked" appearance.
Xerotic dermatitis is more common in older adults, as the skin's ability to retain moisture tends to decrease with age.
Some factors that can contribute to xerotic dermatitis include:
- Cold, dry weather
- Overuse of soaps, detergents, or other harsh cleansers
- Prolonged exposure to water or hot showers
- Medical conditions, such as hypothyroidism or certain genetic disorders
- Use of certain medications that can cause dry skin
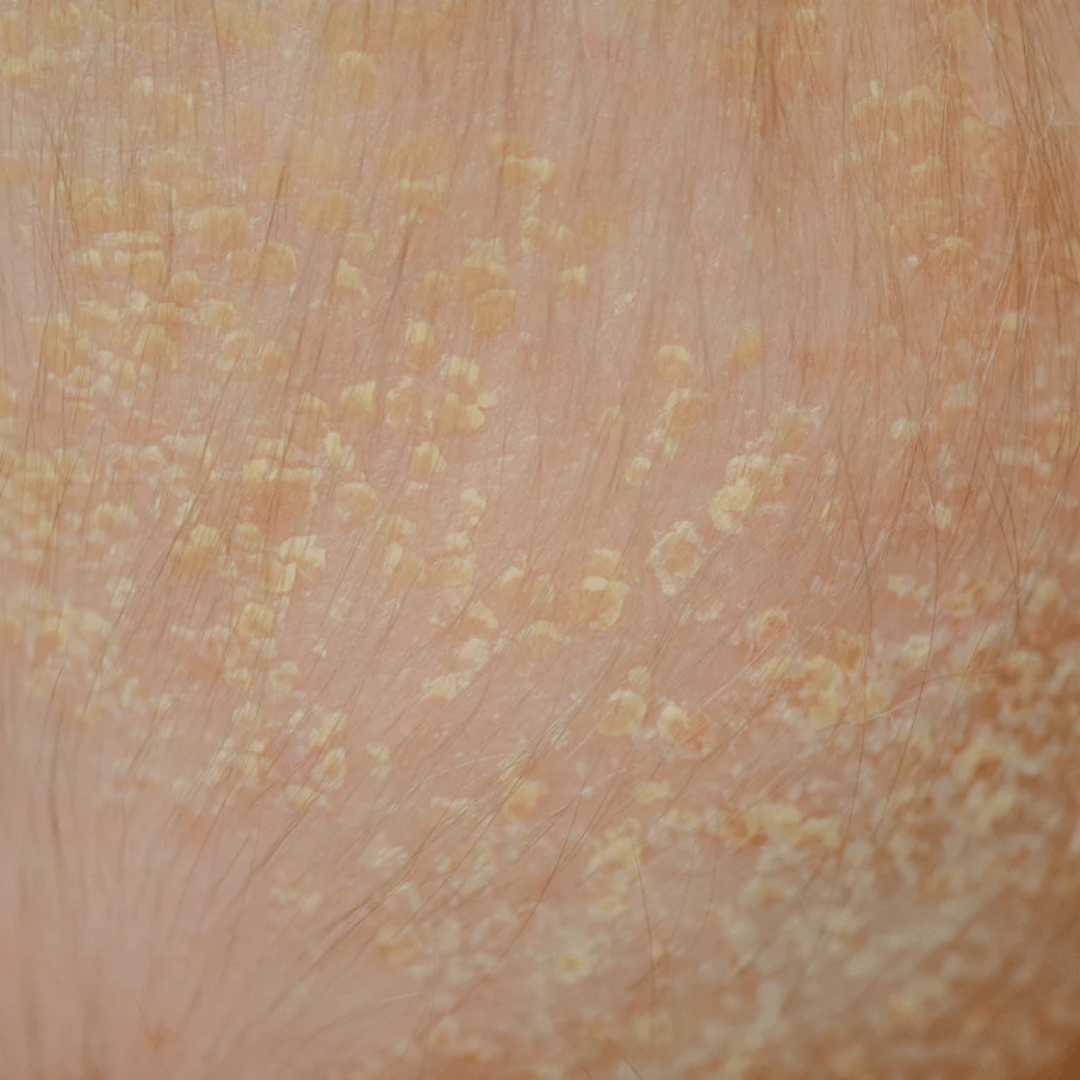
SEBORHEIC DERMATITIS
Seborrheic dermatitis is a common, chronic skin condition that affects areas of the body with a high concentration of oil-producing (sebaceous) glands.
It typically causes red, inflamed, and scaly patches of skin, often accompanied by dandruff. The most commonly affected areas include the scalp, face (particularly around the nose, eyebrows, and ears), and upper chest or back.
The exact cause of seborrheic dermatitis is not fully understood, but it is thought to involve a combination of factors, including:
- Overproduction of sebum (skin oil)
- An abnormal immune response
- The presence of a yeast called Malassezia, which is a normal component of the skin's microbiome but may cause inflammation in susceptible individuals
Seborrheic dermatitis can affect people of all ages but is more common in infants (referred to as "cradle cap") and adults between the ages of 30 and 60.
Topical Steroid Withdrawal
Topical steroids are effective and safe to use in the short-term, but may have more side-effects than benefits if used incorrectly, over a long period of time, or when applied to skin that is very thin such as around the eyes, lips, genital areas and on very young babies and children, for a prolonged period of time, as the absorption increases.
There are a variety of different types and symptoms associated with eczema.
Eczema is an umbrella term often used to describe the relapsing-remitting cycle of dry, itchy, rashy skin.
1. Eczema commonly starts with dry, itchy skin. The scratching is what turns it into the angry, red rash we’re so familiar with.
2. It’s most commonly found in the skin flexures – the elbow patches, knees, neck.
3. It can affect all age groups, but it is most commonly diagnosed before 5 years of age and affects 10% - 20% of kids. About half will outgrow it before adulthood.
4. Diagnosis is primarily clinical and based on symptoms.
5. Atopic Dermatitis is the most common form and is part of the “atopic triad,” along with asthma and allergies.
6. Approximately 70 percent of patients have a positive family history of atopic diseases.
7. Most common triggers: food, stress, irritants, and environmentIncidence of eczema is increasing 2- to 3x in industrialized nations since the 1970s.








